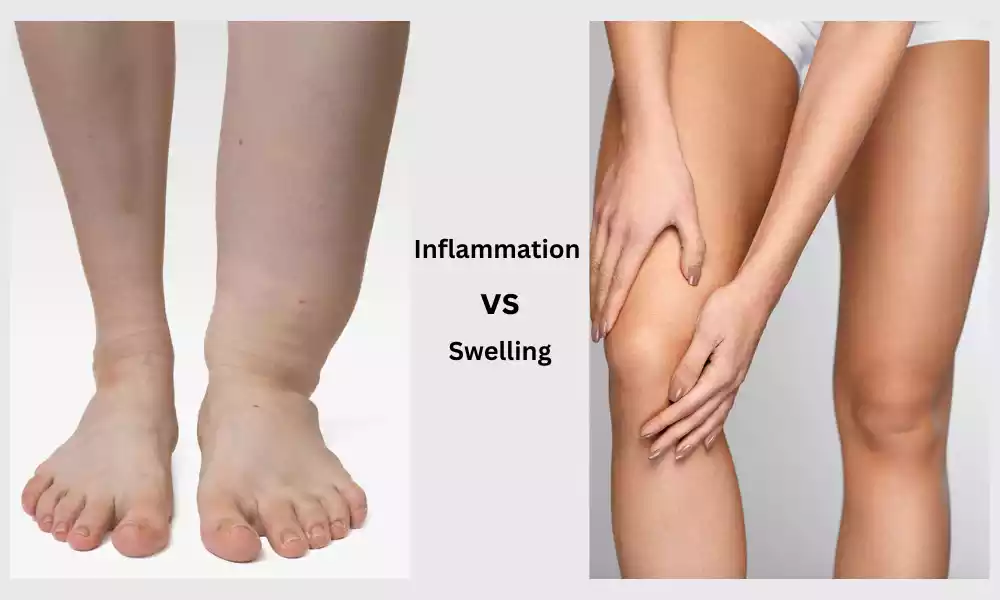
Inflammation and Swelling are normal reactions that our bodies exhibit when confronted with an injury, infection, or other medical circumstances. Although they are often seen in tandem and can be utilized interchangeably, they are distinct biological processes.
Inflammation is the body’s complicated biological reaction to harmful stimuli. It aims to repair and protect the damaged tissue. It’s a series of events that can cause symptoms such as burning, redness, or discomfort. On the other hand, swelling, also known as edema, is the accumulation of fluid inside tissues.
It can be caused by various reasons, including but not only, inflammation itself. Recognizing the differences between these two conditions is vital to ensure a correct diagnosis and efficient treatment.
Definition of Inflammation
Inflammation is a complicated biochemical response in the vascular tissue of your body to negative stimuli such as harmful agents, damaged cells, or irritations. It’s a defense mechanism aimed at eliminating the source of injury to cells to remove necrotic cells and tissues that are damaged due to the initial inflammation and injury as well as initiating the process of tissue repair.
The five most common indicators that indicate inflammation include:
- redness (Rubor): This is due to dilation of blood vessels in the small blood vessels that are located in the area of injury.
- Heating (Calor): Increased blood flow (hyperemia) due to vasodilation results in warmth.
- Splendid (Tumor): This is caused by the increase in fluid.
- The pain (Dolor): Released chemicals and swelling could trigger nerve endings.
- The loss of functionality (Function leakage): In some instances, the inflamed area can be so swollen and painful that it is unable to perform its normal role.
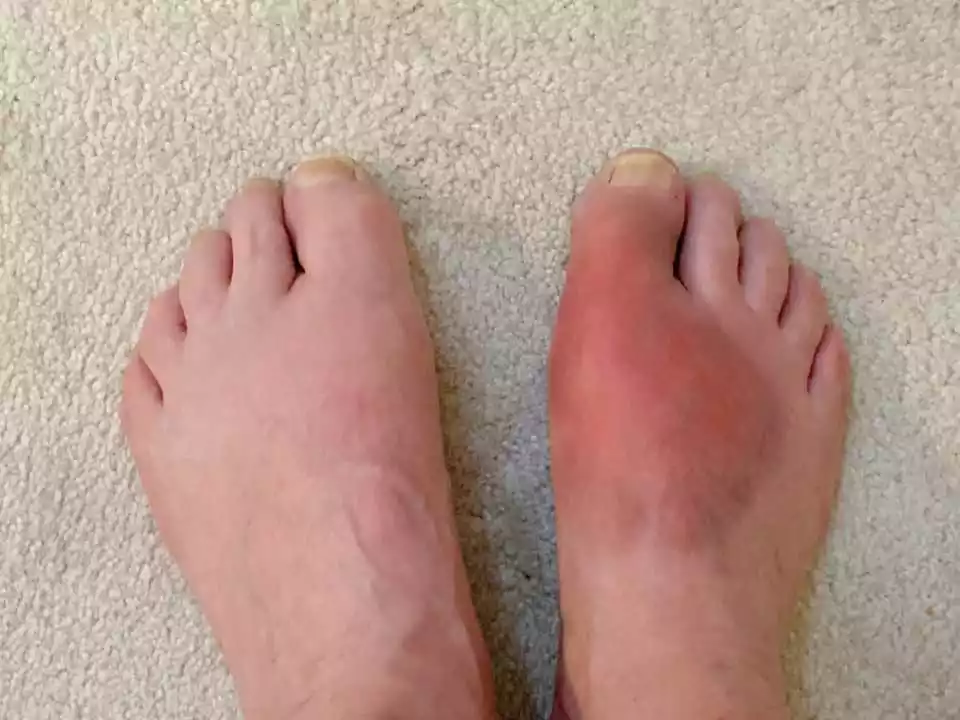
Inflammation can be classified as either chronic or acute. An acute inflammation is a brief procedure that usually manifests in minutes or hours, and is an immediate reaction to injuries. Chronic inflammation however is a long-lasting and continuous inflammatory response that can last for months or even for years.
Definition of Swelling
Swelling, medically known as edema is the expansion or dilation of a part of the body as a result of the accumulation of fluid within tissues. The buildup of fluid can happen due to a variety of reasons and results in the swelling and tightening of the affected region which can cause discomfort or pain.
There are two kinds of edema:
- Pitting Edema If pressure is applied on a swelling region and the indentation, or “pit” remains after the pressure has been released It’s referred to as “pitting edema. This kind of swelling is typically associated with fluid imbalance or circulation.
- Non-pitting Edema If the skin stretches back in a flash without leaving an indentation once the pressure has been applied this is known as non-pitting edema. It can be a result of problems like thyroid disorders or lymphatic obstruction.
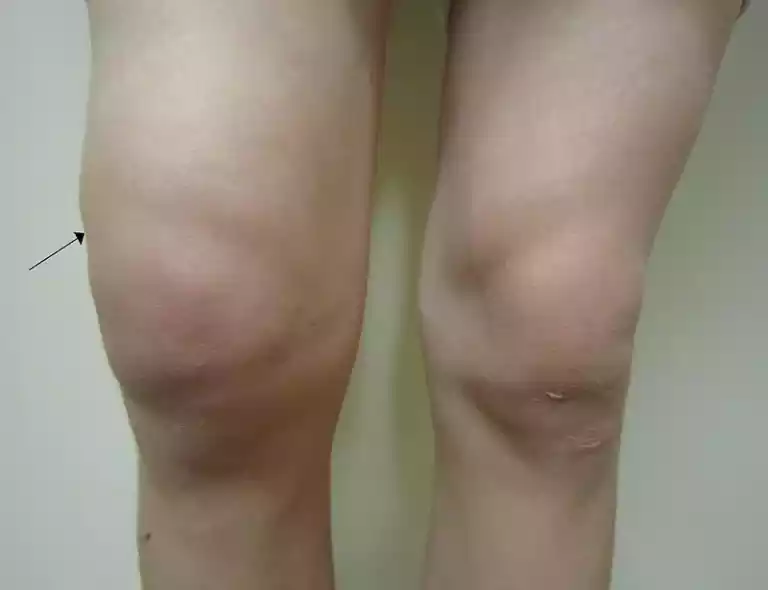
Swelling may occur in particular areas within the human organs (localized) or spread across the body (generalized). The factors that cause swelling vary from common causes for example, like sitting or standing, to more complicated conditions such as kidney failure, heart failure, or inflammation caused by an injury or infection. Understanding the cause of swelling is crucial for proper treatment and management.
Inflammation and Swelling in the comparison chart
Comparison Chart: Inflammation vs. Swelling
| Aspect | Inflammation | Swelling (Edema) |
|---|---|---|
| Definition | A complex biological response of the body’s vascular tissues to harmful stimuli. | Enlargement or distention of an area due to the accumulation of fluid in tissues. |
| Main Causes | – Pathogens (bacteria, viruses, fungi) <br>- Damaged cells or tissues<br>- Irritants | – Fluid buildup due to inflammation<br>- Direct injury or trauma<br>- Circulatory issues<br>- Organ dysfunction (e.g., heart) |
| Symptoms | – Redness<br>- Heat<br>- Pain<br>- Potential loss of function | – Puffiness/enlargement of affected area<br>- Tightness of the skin<br>- Potential pain or discomfort |
| Types | – Acute inflammation<br>- Chronic inflammation | – Pitting edema<br>- Non-pitting edema |
| Diagnostic Tools | – Blood tests (e.g., C-reactive protein)<br>- Imaging (e.g., X-ray, MRI) | – Physical examination<br>- Imaging (ultrasound, MRI)<br>- Measurement of affected area |
| Treatment Modalities | – Anti-inflammatory medications (e.g., NSAIDs)<br>- Corticosteroids<br>- Immune-modulating drugs | – Elevation of the affected area<br>- Compression garments<br>- Diuretics (for fluid retention)<br>- Treating underlying causes |
By observing the distinctions between inflammation and swelling, healthcare professionals can more effectively diagnose, manage, and treat the conditions causing these symptoms.
Causes of Inflammation and Swelling
Inflammation Causes:
Infections:
- Fungal, viral, or parasitic organisms can cause an inflammation response when the body attempts to eliminate or neutralize the pathogen.
Injuries or Trauma:
- Splinters, cuts, scrapes, or burns may result in localized inflammation.
Autoimmune Reactions:
- The immune system of the human body incorrectly attacks its tissues and believes they’re foreign. Examples include rheumatoid and lupus.
Exposure to Toxins:
- Certain chemicals or irritants may cause inflammation if they are in contact with your body.
Chronic Conditions:
- A few conditions, such as Crohn’s disease or asthma can cause chronic inflammation.
External Factors:
- Environmental pollution, ultraviolet radiation as well as extreme weather conditions.
Other Medical Conditions:
-
- Tumors, genetic disorders, or conditions can trigger inflammation.
Swelling (Edema) Causes:
Inflammation:
- In the course of the inflammatory process as part of the inflammatory response, fluids can build up within tissues, causing swelling.
Direct Injury or Trauma:
- Injuries, fractures, or contusions may result in localized swelling.
Fluid Retention:
- The conditions like heart problems, liver disorders, or kidney diseases can lead the body’s system to store more fluid. This can lead to swelling.
Blockage of Fluid Drainage:
- Lymphedema for instance results from a blockage in the lymphatic system.
Medications:
- Certain medications may cause swelling as a side effect such as certain antihypertensives, steroids, and NSAIDs.
Pregnancy:
- Fluid retention is common during pregnancy and is particularly prevalent within the legs.
Chronic Venous Insufficiency:
- Insufficient vein function in the legs causes fluid accumulation and swelling.
Deep Vein Thrombosis (DVT):
- A blood clot that forms in deep veins may cause swelling, usually on one side of the leg.
Other Medical Conditions:
- Thyroid disorders or malnutrition can cause generalized swelling.
While swelling and inflammation may be caused by overlapping causes, especially when it comes to injuries or certain illnesses it is essential to know the subtle distinctions between them to ensure appropriate medical treatment.
Signs and Symptoms of Inflammation and Swelling
Inflammation Signs and Symptoms:
- Redness (Rubor):
-
- The cause is the dilation of tiny blood vessels that are located in the region of injury, causing the area to appear redder than the surrounding tissues.
- Heat (Calor):
-
- The area affected may feel warm because of the increased flow of blood (hyperemia) due to vasodilation.
- Pain (Dolor):
-
- Inflammatory mediators released, such as prostaglandins, may stimulate nerve endings, causing discomfort.
- Swelling (Tumor):
-
- In the event of an increase in the amount of fluid and immune cells in the affected region. This is when swelling and inflammation may overlap.
- loss of function (Function Laesa):
-
- In some cases,, the affected area may be so painful, swollen, and stiff, that the area is unable to maintain its normal function or motion.
- Systemic Symptoms:
-
- In the case of chronic inflammation, the symptoms may include fever, fatigue loss of appetite, and malaise.
Swelling (Edema) Signs and Symptoms:
- Puffiness or Enlargement:
-
- It appears to be larger because of the accumulation of fluid.
- Tightness of the Skin:
-
- The skin can be stretched due to the accumulation of fluid giving it an appearance of shiny or stretched.
- Pain or Discomfort:
-
- The swelling can exert pressure on nearby structures, which can cause the sensation of pain or tightness.
- Reduced Mobility:
-
- If there is swelling in the joint or limb it can cause movement to become restricted.
- Indentation or “Pitting”:
-
- If tension is applied to the area that is swelling the area may create an indentation that lasts for a period of time, especially when there is a pitting edema.
- Weight Gain:
-
- In the case of generalized edema, there could be a rise in body weight because of the retention of fluids.
- Increased Abdominal Size:
-
- If there is swelling within the abdominal area (ascites) It could result in bloating or an expansion of the stomach.
- Stiffness:
-
- Swelling can lead to stiffness in the area affected in particular when it affects joints.
In many instances, swelling and inflammation can be present at the same time, particularly when an infection or injury is the reason. However, knowing the distinct symptoms and signs can aid in the accurate diagnosis and efficient treatment plans.
How they Interrelate
How Inflammation and Swelling Interrelate
Swelling and inflammation (edema) both are manifestations of the body. They are often seen in conjunction, especially in the aftermath of infection, injury, or other medical circumstances. To comprehend their relation it is necessary to understand the mechanisms that trigger each of the phenomena.
- Initiation of Inflammation:
-
- When tissues become damaged or when pathogens from outside invade the body, a rapid response is activated. This reaction triggers the release of several chemical mediators like histamines, bradykinin, and prostaglandins. These mediators increase vasodilation which improves the flow of blood to the area affected, resulting in redness and warmth frequently associated with inflammation.
- Swelling as a Result of Inflammation:
-
- One of the consequences of the increase in blood circulation and permeability of the vascular system when there is inflammation is the leakage of fluid into interstitial space (spaces between cells). The accumulation of fluid within tissues causes an increase in swelling. It is known as edema. Therefore, in many instances, swelling is an immediate result of inflammation.
- Role of White Blood Cells:
-
- In the course of an inflammation response As part of the inflammatory response, white blood cells are drawn to the location of the injury or infection. They move out of blood vessels to the tissues affected and are referred to as Chemotaxis. Their presence, together with other cells, contributes to the swelling.
- Prolonged Inflammation and Chronic Swelling:
-
- If the root of inflammation isn’t removed, the inflammation could develop into chronic. Chronic inflammation can result in chronic swelling, and damaged tissue, and could contribute to the onset of conditions such as rheumatoid arthritis, where joints become painful and swollen for long durations.
- Swelling Without Inflammation:
-
- It is important to remember that, while inflammation can result in swelling, it’s not every swelling is caused by inflammation. The swelling could be due to different causes, like lymphatic obstruction, excessive fluid due to heart failure, or direct traumatic injury. In these cases, the swelling may not be accompanied by typical signs of inflammation such as heat, redness, or discomfort.
- Therapeutic Interventions:
-
- Many therapies, such as nonsteroidal anti-inflammatory medications (NSAIDs) have the goal of helping decrease inflammation as well as the swelling that results. The use of compression garments, elevation, and cold compresses may be used to help reduce swelling.
In the end, swelling and inflammation are entwined in a way and the latter often results in the latter. However, they can happen independently, and knowing the difference between them is vital for diagnosing and treating them.
What complications if Inflammation and Swelling are Left Untreated?
Complications of Untreated Inflammation:
- Chronic Inflammation:
-
- If inflammation that is acute is not removed, it could turn into a chronic one that may last for months or even a decade. Chronic inflammation is associated with many health conditions.
- Tissue Damage:
-
- The instability that persists can lead to tissue destruction or damage. For example, in cases such as rheumatoid arthritis inflammation can cause joint tissue to break down.
- Scarring:
-
- Inflammation in organs such as the lung or liver can cause scarring (fibrosis) that can affect organ function.
- Development of Diseases:
-
- Chronic inflammation can be linked to many diseases, including cancer, heart disease diabetes, as well as neurodegenerative disorders such as Alzheimer’s disease.
- Compromised Immune Response:
-
- Chronic inflammation can result in weakening the immune system, which makes the body more vulnerable to illness or infections.
- Systemic Effects:
-
- Chronic inflammation can trigger general symptoms such as fatigue, weight loss, and fevers.
Complications of Untreated Swelling (Edema):
- Pain and Discomfort:
-
- As the swelling increases it will cause the skin to stretch and put pressure on nearby structures which can cause pain and discomfort.
- Impaired Circulation:
-
- The swelling can hinder the circulation of blood to the area, which can lead to complications such as blood clots.
- Stiffness and Reduced Mobility:
-
- The constant swelling of areas such as joints can limit motion and result in stiffness.
- Skin Breakdown:
-
- The prolonged swelling could result in the skin’s stretch and itchy. It is also vulnerable to breakdown, possibly causing infections or ulcers.
- Scarring:
-
- Edema that has been present for a long time can cause tissues that are fibrotic which can lead to scarring.
- Compartment Syndrome:
-
- It’s a serious problem wherein swelling in muscles can increase pressure and block blood flow, which could cause nerve and muscle damage. It’s regarded as a medical emergency.
- Pulmonary Edema:
-
- If there is swelling in the lung, this could cause breathing difficulties and reduced oxygenation, which is a possible life-threatening condition.
- Ascites and Organ Dysfunction:
-
- The abdominal cavity is swelling (ascites) caused by diseases like liver disease could cause organ dysfunction and can result in complications such as peritonitis bacterial.
Inflammation and swelling function as the body’s reaction to abnormal or traumatic conditions. If they are not addressed and treated correctly, they can cause more serious health problems. The early detection of these issues and the appropriate treatment are essential to avoid these potential problems.
Diagnostic Approaches
Diagnostic Approaches for Inflammation and Swelling
For Inflammation:
- Physical Examination:
-
- The affected area is examined for the classic signs of inflammation including heat, redness, swelling, pain or loss of functioning.
- Blood Tests:
-
- Certain blood tests could be a sign of inflammation within the body:
-
-
- Complete Blood Count (CBC): This may reveal an increased white blood cell count, which can indicate an infection or inflammation.
- Erythrocyte Sedimentation Rate (ESR): A non-specific test that can reveal that there is inflammation.
- C-Reactive Protein (CRP): A liver-produced protein as a response to inflammation.
- Additional specific indicators: Depending on the suspected illness the other markers such as antinuclear antibodies or rheumatoid factor could be tested.
-
- Imaging Studies:
-
- X-rays: Could reveal the changes that occur in joints or bones caused by chronic inflammation.
- MRI as well as CT Scans: They provide detailed pictures and assist in identifying the areas that are inflamed within soft tissue.
- Ultrasound: A useful tool for diagnosing inflammation structures that are superficial like joints or tendons.
- Biopsy:
-
- In certain instances, a small amount of the tissue may be taken from an area affected to be scrutinized under a microscope to detect evidence of inflammation as well as other signs of abnormalities.
For Swelling (Edema):
- Physical Examination:
-
- Evaluation of the swollen region Check the area for any pitting (where the skin remains with an indentation after having been pressed).
- Measurement:
-
- It is the size and shape of the swollen region can be measured to monitor the changes in time.
- Blood Tests:
-
- To identify any conditions which can cause swelling, for example, liver or kidney function tests.
- Urine Tests:
-
- Can be used to look for proteinuria (excess urine protein) This is an indication of kidney issues.
- Imaging Studies:
-
- X-rays: Could reveal the accumulation of fluid or other abnormalities in joints and bones.
- MRI as well as CT scans: They provide clear images of the soft tissue as well as reveal areas of accumulation of fluid.
- Ultrasound: is Used to assess swelling in the superficial structures. It may also aid in identifying blood clots or fluid accumulations.
- Doppler Ultrasound: The ability to measure blood flow, and detect blood clots that are present in veins.
- Lymphoscintigraphy:
-
- A special imaging test will evaluate the functioning that the lymphatic system performs as well as determine conditions such as lymphedema.
- Cardiac Evaluation:
-
- When heart problems are believed to be an underlying cause for swelling, tests such as echocardiography may be used to evaluate the function of the heart.
Both swelling and inflammation are signs that may have multiple root causes. Therefore, the approach to diagnosis is usually multifaceted and aims to determine both the presence and the cause to determine the best treatment.
Treatment Modalities of Inflammation and Swelling
For Inflammation:
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs):
-
- Examples: Ibuprofen, naproxen, aspirin. They reduce inflammation and pain by blocking enzymes that are involved in the inflammatory process.
- Corticosteroids:
-
- Effective anti-inflammatory medications that are ingested and applied as creams or injected. Examples include cortisone or prednisone.
- Biologics:
-
- These are drugs that are based on proteins and that are derived of living cells. They target specific regions in the immune system, reducing inflammation. They are particularly effective in treating autoimmune diseases such as rheumatoid arthritis. Some examples include adalimumab (Humira) along with infliximab (Remicade).
- Disease-Modifying Antirheumatic Drugs (DMARDs):
-
- For rheumatic conditions, it is recommended to slow their progression and protect the joints and other tissues from long-term destruction.
- Physical Therapy:
-
- Maintains joint function and reduces inflammation by performing specific exercises and treatments.
- Rest and Joint Protection:
-
- Letting the affected area rest will help in reducing inflammation. Braces or splints can be employed to guard joints.
For Swelling (Edema):
- Elevation:
-
- Lifting the affected limb above the heart may help to decrease swelling.
- Compression:
-
- Bandages or compression stockings can aid in reducing and preventing the accumulation of fluids in tissues.
- Diuretics (Water Pills):
-
- They aid the body in getting rid of extra fluid and salt by urination.
- Massage:
-
- The manual lymphatic drainage method, which is a specific type of massage, may aid in the removal of fluid from areas that are swollen.
- Physical Therapy:
-
- Therapists can help patients with exercises that assist in improving the drainage of fluids.
- NSAIDs:
-
- Although these may help to reduce swelling, it’s important to remember that they may also cause swelling. Always consult a medical expert prior to using.
- Surgery:
-
- If swelling occurs due to obstructions or structural problems, surgery may be an alternative.
It’s crucial to keep in mind that the treatment option you select will be determined by the root reason for the swelling or inflammation. It’s crucial to collaborate with medical professionals in determining the most effective treatment strategy for the specific circumstances.
Furthermore, some treatments may cause adverse reactions or possible interactions It’s essential to be well-informed and monitored when you are using these treatments.
Prevention Strategies of Inflammation and Swelling
General Prevention Strategies:
- Healthy Diet:
-
- Eat a balanced and balanced diet that is rich in antioxidants and omega-3 fatty acids and anti-inflammatory foods like fish, berries and berries olive oil, nut and green leafy vegetables, and whole grains.
- Limit or eliminate the consumption of processed food items, sugary drinks, and excessive consumption of red meat.
- Maintain a Healthy Weight:
-
- Being overweight can trigger inflammation and place extra strain on joints, thereby increasing the chance of swelling.
- Regular Exercise:
-
- Physical activity can help decrease inflammation and increase circulation, which helps reduce swelling.
- Make sure to do exercises with low impact, especially when you are prone to joint pain.
- Stay Hydrated:
-
- Drinking plenty of water can rid the body of toxins. This will reduce the chance of inflammation.
- Limit Salt Intake:
-
- Salt intake can cause swelling and retention of fluid particularly in people who are who are sensitive to salt.
Specific Prevention Strategies for Inflammation:
- Avoid Tobacco and Limit Alcohol Consumption:
-
- Drinking alcohol and smoking cigarettes can cause inflammation.
- Regular Health Screenings:
-
- Early detection and treatment of health issues can help prevent chronic inflammation.
- Stress Management:
-
- Stress can cause chronic inflammation. Meditation, yoga as well and deep breath exercises, can ease stress.
- Proper Dental Hygiene:
-
- Periodontal problems can cause inflammation, which is why regular dental examinations and good dental hygiene are vital.
Specific Prevention Strategies for Swelling (Edema):
- Elevate Legs:
-
- If you sit for long durations, lift the legs to avoid the accumulation of fluid.
- Avoid Standing for Long Periods:
-
- Long-term standing can cause an accumulation of fluid in the legs.
- Wear Supportive Shoes and Compression Garments:
-
- This will increase circulation and lower the possibility of swelling particularly in cases of edema.
- Avoid Tight Clothing:
-
- The restriction of clothing can hinder circulation and cause swelling.
- Move Regularly:
-
- On long flights and drives, you should try to walk or run around frequently to avoid the build-up of fluids.
- Monitor Medications:
-
- Certain medications may cause swelling as an adverse result. If you notice swelling following beginning a new drug you should consult a medical expert.
Prevention is typically the best option for controlling swelling and inflammation. Embracing a healthy way of life, making informed decisions and regular consultation with medical professionals can greatly lower the chance of developing these ailments.
Conclusion
Swelling and inflammation are the natural responses of the body in response to an injury, infection, or other ailment. While they are essential in the healing process and protect against harm If they are not addressed or controlled, the occurrences could cause complications and discomfort.
Knowing the causes, differences, and treatments that are possible is crucial. By taking proactive measures, and consulting out timely health advice we will be able to more effectively manage these ailments and enhance overall well-being.
Being aware and taking proactive actions are essential in ensuring that the body’s protection mechanisms are working to protect us instead of against us.