Agglutinogens and Agglutinins: Agglutinogens and Agglutinins differ in that an agglutinogen is any antigen or foreign body that triggers the production of antibodies in our immune system, while antibodies themselves are produced from our own bodies as agglutinins.
Agglutination refers to the formation of aggregates by antibodies reacting with antigens. This process includes two stages, initial binding or sensitization and lattice formation. Agglutination serves as an immune response that removes pathogenic substances and microbes from our bodies; an agglutination test can help detect pathological entities as well as blood groups.
Definition of Agglutinogens
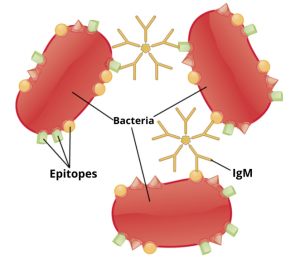
Red blood cells or other cells contain antigens that play an essential role in determining one’s blood type. Aglutinogens play the most notable role, distinguishing A, B and Rh blood groups and contributing to their formation by inheritance or individual genetic differences; the presence or lack of certain agglutinogens affect an individual’s type of blood and compatibility for transfusions.
Agglutinin Definition
Agglutinins, or antibodies, are produced by our bodies when foreign agglutinogens on red blood cells or other cells are detected. Agglutinins (IgM and IgG antibodies that bind agglutinogens) are immunoglobulins that recognize and bind specific agglutinogens leading to their process of clumping or agglutination; their immune response can have profound effects when transfusing blood; these agglutinins influence blood typing as well as transfusion medicine; when blood transfused against incompatible antigens they may cause red cells to clump, potentially leading to potentially harmful reactions.
Importance of understanding the difference between agglutinogens and agglutinins
Understanding the difference between agglutinogens (agglutinins) and agglutinins for blood transfusion medicine is critical to safe and successful transfusions. To maximize safety and efficacy, donor blood agglutinogens must match up with any antibodies absent in recipient plasma to avoid adverse reactions such as hemolysis or agglutination that might otherwise arise during transfusions.
Immunological Investigations: Agglutinogens, agglutinins, and other components are an integral part of many serological tests used to diagnose and treat various diseases. Their interaction is at the foundation of various tests such as cross-matching and antibody screening – their roles and properties must be fully understood in order to accurately interpret test results and make informed clinical decisions.
Hemolytic disease in newborns: To effectively prevent and treat Hemolytic Dialysis of Newborns (HDN), it is crucial that we recognize the difference between agglutinogens (agglutinins) and agglutinins for treatment purposes. Maternal agglutinins that do not match up well with fetal red cell agglutinogens can cross membrane barriers and damage red cells directly; so it is crucial that we recognize and manage any incompatibilities to avoid severe complications for newborns.
Studies and scientific understanding: Establishing the distinction between agglutinogens and agglutinins in immunology is critical for creating diagnostics and therapies, while understanding their interactions and properties is necessary for furthering science, optimizing lab techniques and designing targeted interventions.
Understanding the difference between agglutinogens (agglutinins) and agglutinins will enable you to accurately type blood, ensure safe transfusions for patients, diagnose blood-related disorders effectively, and avoid adverse reactions.
Agglutinogens
Antigens found on red blood cells or other cells play an integral part in determining one’s blood group. Aglutinogens play a critical role in distinguishing different blood types such as A, B and Rh. Their antigenic properties define each blood type’s characteristics, such as A-B-Rh classification. Affected RBCs either possess specific antigenic proteins known as antigens that determine one’s antigenic profile as well as compatibility for transfusion.
Agglutinins
Agglutinins, or antibodies, are produced by our immune systems when foreign agglutinogens appear on red blood cells (or other cells). Agglutinins – IgM and IgG antibodies that bind specific agglutinogens – act like immunoglobulins in that they recognize specific agglutinogens which ultimately leads to their clumping together and eventual clumping off, potentially compromising blood transfusion safety and making transfusion medicine more complicated.
Differences Between Agglutinogens & Agglutinins
There are a few key distinctions between agglutinins and agglutinogens, which have the following key features:
Nature:
Agglutinogens: Agglutinogens are antigens present on red blood cells and other cells, providing antigenic properties specific to particular blood types.
Agglutinins: Agglutinins (or antibodies) are produced as part of an immune response to certain agglutinogens; specifically immunoglobulins like IgM and IgG antibodies.
Locate:
Agglutinogens can be found on the surfaces of red blood cells and other cells.
Agglutinins can be found in plasma or serum (the liquid component of blood).
Role:
Agglutinogens play an essential part in determining an individual’s blood type and compatibility; additionally, they cause the agglutination reaction seen during blood type tests or transfusions.
Origin:
- Agglutinogens may be passed down from one parent to the next through genetic inheritance; their existence being determined by DNA analysis.
- Your immune system produces agglutinins as a protective response against foreign agglutinogens like those found through transfusions or vaccinations.
Specificity:
- Each blood type has its own specific Agglutinogens that can be classified according to different systems, such as ABO and Rh. They each possess antigenic properties unique to themselves and should be carefully considered when making medical decisions.
- Agglutinins recognize specific agglutinogens. Anti-A antibodies, for instance, specifically recognize A and B antigens in ABO blood typing systems.
- Understanding these distinctions is integral to blood typing, compatibility with transfusions and accurately interpreting serological tests. Agglutinogens determine your blood type; while agglutinins determine immune reactions and transfusion compatibility.
Table difference:
| Aspect | Agglutinogens | Agglutinins |
|---|---|---|
| Definition | Antigens found on the surface of red blood cells or other cells | Antibodies produced by the immune system in response to agglutinogens |
| Location | The surface of red blood cells or other cells | Present in the plasma or serum |
| Role | Determine an individual’s blood type and compatibility | Bind to agglutinogens, causing agglutination reactions |
| Origin | Inherited from parents | Produced by the immune system in response to exposure |
| Nature | Antigens | Antibodies |
| Specificity | Each blood type has specific agglutinogens | Agglutinins are specific to the agglutinogens they recognize |
Relationship Between Agglutinogens & Agglutinins
Agglutinogens and Agglutinins can be related in this manner:
Agglutinins – antibodies – recognize and bind to agglutinogens present on red blood cells and other cells’ surfaces, creating immune complexes in response.
Agglutination reaction: When two agglutinins and agglutinogens combine, their binding produces a series of reactions that lead to cell clumping or “agglutination.” This phenomenon can be observed visually during laboratory tests; its significance lies in blood typing and compatibility evaluation.
Blood Typing: Agglutinogens can be used to determine an individual’s blood type and compatibility for transfusion purposes. Under the ABO system of blood typing, for example, the presence or absence of AGGlutinogen A or B indicates type A blood and B blood respectively; anti-A and anti-B antibodies can also be detected in plasma samples from those without the relevant antigens present.
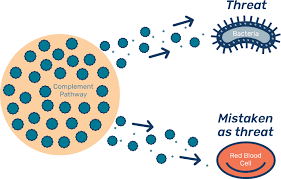
Immune Response: When exposed to foreign agglutinogens, our immune systems produce agglutinins as an immune response and protect our bodies from potential threats such as incompatible transfusions or foreign substances entering the bloodstream.
Compatibility of Blood Transfusions: Compatibility in transfusions is determined by ensuring there are no mismatched agglutinins between red blood cells of a donor and plasma from their recipient that could result in hemolysis or agglutination, and such complications could even be life-threatening.
Understanding the relationship between agglutinogens, agglutinins, and their cross-matching is paramount for safe blood transfusions, blood typing and cross-matching. Compatibility occurs when recipient blood plasma does not react with donor red cells in terms of agglutinogens; thus preventing agglutination and guaranteeing successful transfusion.
Clinical Significance / Implications W. B. Grossin
Hemolytic transfusion reactions: Hemolytic reactions can occur due to incompatible agglutinogens or agglutinins, when transfusing red blood cells are destroyed through reactions between donor-derived agglutinogens and those from recipient blood, thus leading to red cell destruction (hemolysis). Mild or severe, life-threatening reactions have occurred from this reaction; to reduce it further, it is crucial that any used transfusion matches both donor and recipient blood’s agglutinin levels as an initial step in matching these components in exchange transfusions. To minimize such reactions it is vitally important that donors and recipients alike match both donors/donors used during blood transfusions before proceeding with blood transfusions involving donor/donor blood transfusions.
HDN: Hemolytic Disease of the Newborn (HDN) occurs due to an incompatibility between red blood cell agglutinogens found on fetal red blood cells and maternal plasma agglutinins, specifically when carrying a baby of one Rh-negative mother carrying another of different Rh type. When carrying a Rh-positive baby, maternal immune systems produce antibodies that attack red blood cells in fetal bodies causing hemolysis; this condition may result in severe anemia as well as other serious health complications for newborns.
In order to minimize or reduce these incompatibilities it is crucial that pregnant mothers identify and manage these incompatibilities so as not to affect either mother or her baby during gestation or birth. To minimize or minimize HDN effects it is important for mothers to recognize and manage any potential incompatibilities so as not to affect either effects it occurs or minimize its effects upon birthing.
Blood Typing and Cross-Matching: For effective blood typing and cross-matching procedures, it is crucial that one understands the differences between agglutinogens (agglutinins) and agglutinins in order to successfully carry out these processes. Cross-matching involves the process of determining whether specific agglutinogens (red blood cells) and their counterpart agglutinins (plasma). To ensure safe and compatible transfusion procedures it is imperative that both sets are accurately identified and matched –
Diagnose and Treat Blood Disorders: Agglutinogens, agglutinins, and other blood-related substances play an essential role in diagnosing and treating various blood disorders. Their presence can be detected via serological tests that screen for antibodies as part of diagnosis as well as conditions like autoimmune hemolytic anemia, hemolytic diseases of the newborn, transfusion reactions or even transfusion reactions. Understanding their interactions helps interpret test results more precisely as well as provide appropriate medical interventions.
The difference between agglutinogens and agglutinins can have significant clinical ramifications when it comes to preventing transfusion reactions that result in hemolysis, the management of HDN, accurate blood typing, and diagnosing blood disorders. Understanding their relationship is integral for safe and effective patient treatments in immunohematology/transfusion medicine.
Conclusion
In short, agglutinogens as well as agglutinins have a role to play with respect to blood compatibility, immune reactions and so on. Agglutinogens, or antigens, are found in red blood cell surfaces, which determine the blood type of an individual and agglutinins are the antibodies that are produced in reaction to foreign antigens, which include those that are that are found within red blood cell membranes. Understanding the interaction between these components is vital for safe blood transfusions. It aids medical professionals to better manage immune reactions in various clinical scenarios.

